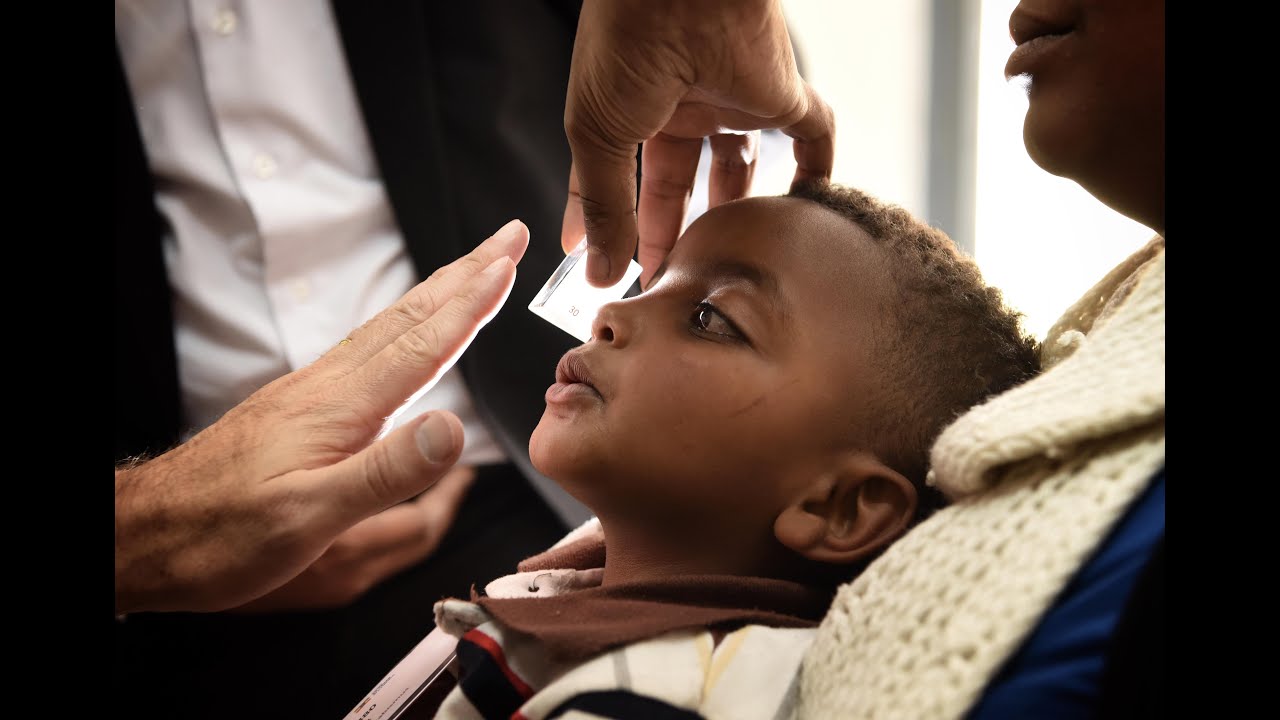
When we started working in Ethiopia in 1998 the population was around 65 million. Two decades later it has nearly doubled to 107 million. According to the World Health Organisation (WHO), over 1.6 million or 1.6% of the Ethiopian population is blind and 3.8 million or 3.7% live with low vision. This falls significantly above the world average of 1.2% and 3.4% respectively.

Ethiopia
Four million people in Ethiopia are blind or visually impaired. Cataracts are the leading cause, affecting some 1.7 million people. The country also accounts for 30% of trachoma in sub-Saharan African countries, or 1.2 million people. With only 140 ophthalmologists in the country, there is a severe shortage of eye health professionals.
The Problem

Five million
people suffering from blindness or vision loss

91%
of low vision is treatable

40%
of children between 1-9 years old have active trachoma
Success in Ethiopia
In 1998 the country had just 54 ophthalmologists, 42 of whom practised in Addis Ababa (the capital city). There are now 140 ophthalmologists.
We have played a leading role in developing 266 primary eye care units, 10 secondary eye care units, 3 paediatric eye care centres and 6 optical workshops.
We've delivered more than 3 million eye screenings and examinations and nearly 25 million medical treatments including around 230,000 surgeries for adults and nearly 9,000 for children
In 2020 alone, we delivered:

21,000
trainings for eye care
professionals

145,000
patients accessing eye care services

86,000
community eye screenings and examinations

7.5 million
doses of antibiotics for trachoma
With your continued support, we can implement a model for comprehensive rural eye care that addresses critical gaps through capacity building, healthcare technology and advocacy. We will train more community health care workers in all aspects of eye care, from awareness of services, identification, diagnosis, referral and treatment.
We will look to face the enormous challenge of trachoma in Ethiopia by implementing the World Health Organisation's SAFE strategy (eyelid surgery, antibiotics, face cleanliness and environmental improvement). We will continue to help reduce the risk of trachoma by training nurses to perform trichiasis surgeries at primary healthcare units and building awareness by teaching community health workers, teachers, local women’s group leaders and community leaders about eye health.
What We're Doing Next
We have enjoyed great successes in Ethiopia over the past 20 years but there is still a huge amount of work to be done to further improve the quality of eye care:
We must do more if we are to help Ethiopia reach its target of eradicating blinding trachoma by 2020. While we are succeeding in reducing the spread of infection in our current regions, we need to take on more districts to expand our trachoma elimination and SAFE strategy roll out. That means we need to secure more funding to expand and cover the whole more of the country.
Ethiopia is in desperate need of more qualified ophthalmologists. Currently there are only five academic institutions offering 25 residents in ophthalmology training each year - this is simply not enough to fight blindness in the country.
We need further support to train the next generation of eye health specialist as we invest in training programs. The doctors we have trained over the past 20 years are now the teachers and we need to create more homegrown opportunities to train the next generation of eye health professionals.
We face the enormous challenge of trachoma in Ethiopia by implementing the World Health Organisation’s SAFE strategy (eyelid surgery, antibiotics, face cleanliness and environmental improvement). We continue to help reduce the risk of trachoma by training nurses to perform trichiasis surgeries at primary healthcare units and build awareness by teaching community health workers, teachers, local women’s group leaders and community leaders about eye health.
We have a long-standing partnership with the Federal Ministry of Health, through which we work to develop and strengthen the capacity of existing government health providers to deliver eye care services at all levels.
Partners
- Federal Ministry of Health
- The Charities and Societies Agency
- Regional Health, Education, Finance and Economic Development Bureau
- District level sector offices
- ICTC
- NCBP